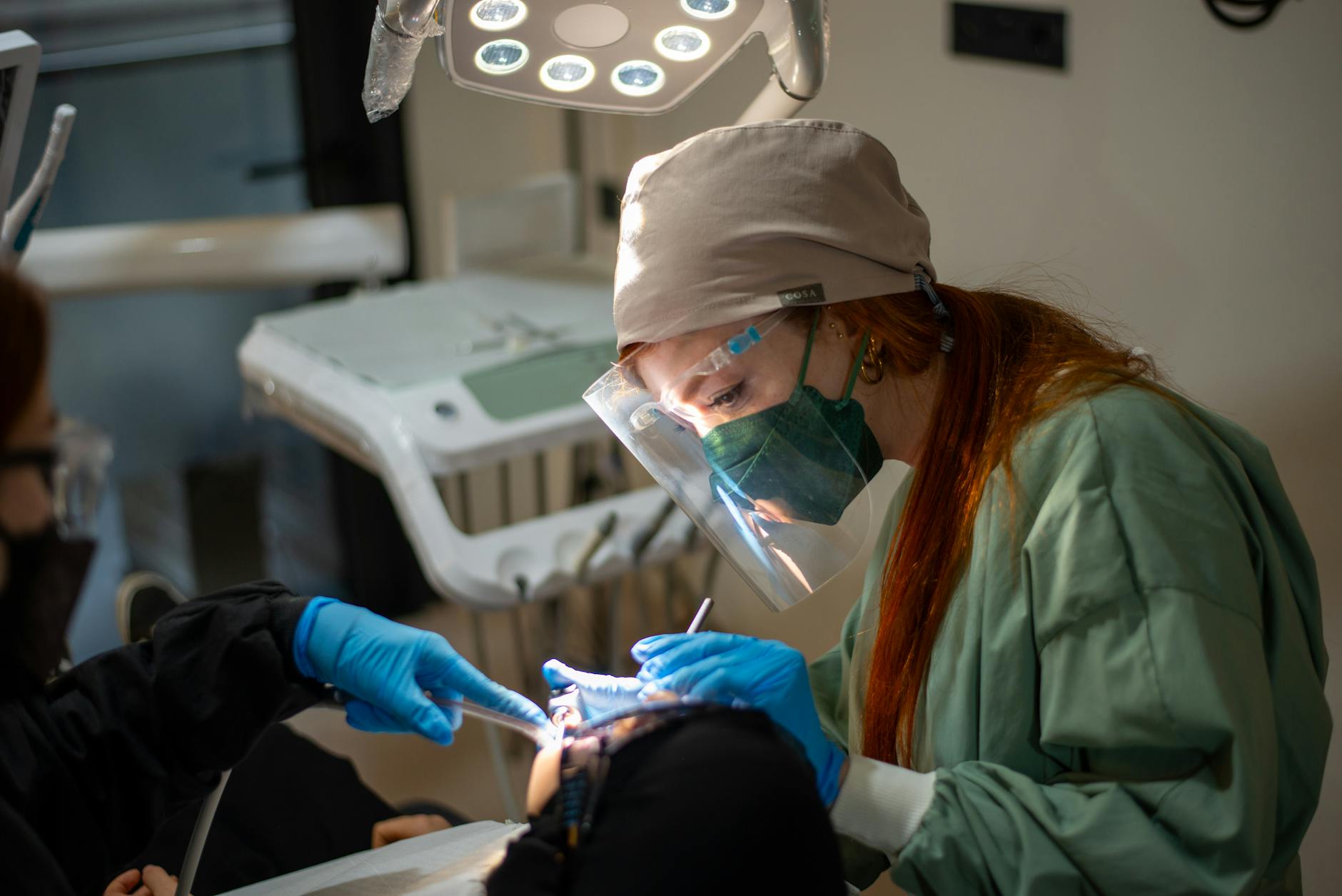
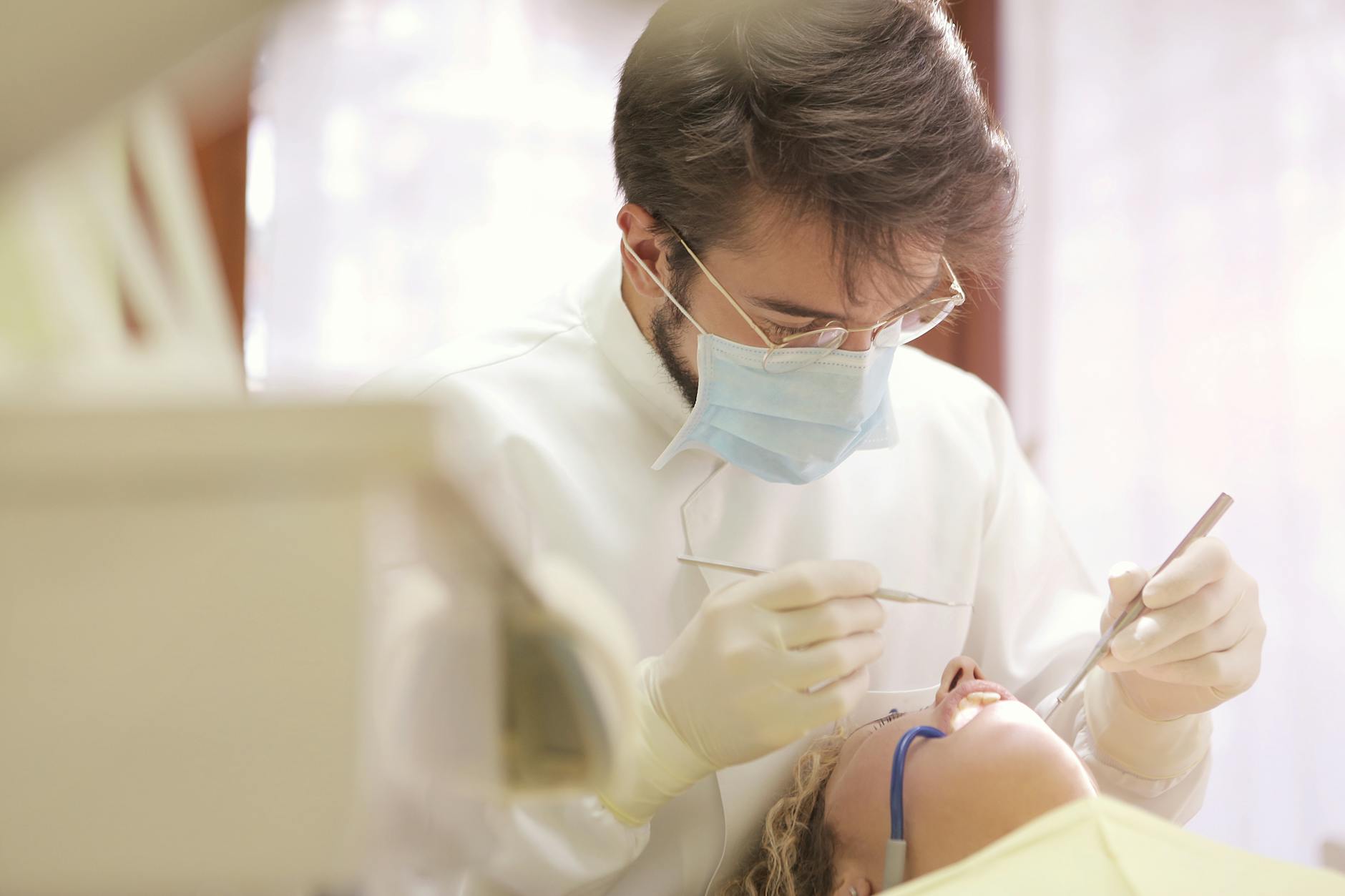
Understanding Tooth Extraction
Tooth extraction is the careful removal of a tooth from its socket when a tooth can’t be predictably restored or is causing pain, infection, or crowding. In our Glendale office, we prioritize saving teeth when possible, but if removal is the safest path, we explain each step and what normal healing looks like. If you’re looking for an extraction healing timeline, it helps to know that healing begins with a protective blood clot in the socket, followed by gradual repair of gum and bone.
During an extraction, the area is numbed and you’ll feel pressure, not sharp pain; afterward, a gauze pad helps the clot form. The first 24 hours focus on protecting that clot: rest, keep your head elevated, bite gently on fresh gauze as directed, avoid spitting or using straws, and stick with soft, cool foods and small sips of water. Swelling and mild oozing can be normal; a cold compress on the cheek in short intervals can help. After the first day, you can start gentle saltwater rinses and resume brushing carefully, avoiding the socket; take only over‑the‑counter pain relievers as directed unless your dentist advises otherwise. Everyone heals at a different pace, but most people notice early tenderness improve over several days while the gums continue to close over the site in the weeks that follow. If you think a tooth might need to come out, we can examine it and discuss options, including emergency tooth extractions, during our business hours (9:00am–5:00pm Mon–Thu; 9:00am–2:00pm Fri). When to call now: if you have severe pain that isn’t improving, heavy bleeding, fever, or increasing facial swelling, please call our Glendale office during business hours for guidance and a prompt evaluation.
Extraction Healing Timeline Overview
Here’s what most people can expect after a tooth is removed, so you can tell what’s typical and when to check in with us. The extraction healing timeline varies by which tooth was removed, how complex the procedure was, and your overall health, but the general pattern is fairly consistent. We’re here to guide you through recovery and answer questions during our office hours (9:00am–5:00pm Mon–Thurs, 9:00am–2:00pm Fri).
- First 24 hours: A blood clot forms in the socket; light oozing is common. Rest, keep your head elevated, bite gently on clean gauze as directed, and use a cold compress in short intervals to help with swelling.
- Days 2–3: Swelling and soreness usually peak around 48–72 hours, then begin to improve. Stick to soft, cool-to-lukewarm foods and begin gentle saltwater rinses after the first day if you were advised to rinse.
- Days 4–7: Discomfort generally eases, and any bruising starts to fade. Keep the area clean with careful brushing around the site; avoid straws and smoking so you don’t disturb the clot.
- Week 2: Gum tissue continues to close over the socket and tenderness decreases. Gradually return to a normal diet as comfort allows, but avoid hard or seedy foods that can lodge in the area.
- Weeks 3–4 and beyond: The surface looks and feels better, while bone under the gum continues to fill in over the next several weeks to months. If you’re planning next steps (like replacing the tooth), we’ll advise you on appropriate timing at a follow-up.
Healing isn’t identical for everyone—if pain suddenly worsens after it had started improving, if you notice increasing swelling, ongoing bleeding, fever, or a persistent bad taste or odor, please call our Glendale office so we can assess you in person. For comfort questions between visits, you can also review our guidance on emergency tooth pain relief; if concerns remain, we’ll schedule you during business hours (9:00am–5:00pm Mon–Thurs, 9:00am–2:00pm Fri). When to call now: contact us immediately during business hours if you have heavy bleeding that won’t slow, facial swelling that’s getting worse, or pain that’s severe and unrelieved by recommended measures.
When to Call a Dentist
After a tooth extraction, mild soreness, swelling, and a small amount of oozing are common during the first couple of days. Call a dentist if your symptoms are not easing along the expected extraction healing timeline, or if anything feels suddenly worse rather than steadily improving. It’s better to have changes assessed during business hours than to wait and hope they pass. Our Glendale team answers calls Monday–Thursday 9:00am–5:00pm, and Friday 9:00am–2:00pm.
Reach out promptly if bleeding continues to soak gauze after firm pressure for 30–60 minutes, if pain intensifies after day two or keeps you from sleeping, or if you notice a persistent bad taste or odor, a visibly empty-looking socket, or dark clot that seems dislodged. Call if you develop fever or chills, swelling that increases after 48–72 hours or spreads to the face or under the jaw, ongoing numbness or tingling after the anesthesia should have worn off, pus or drainage, or trouble opening your mouth, swallowing, or speaking due to discomfort. Until you’re seen, you may place clean, folded gauze and bite gently to help control minor oozing, apply a cold compress on the cheek in short intervals, keep your head elevated when resting, and use over‑the‑counter pain relievers as directed if safe for you; avoid vigorous rinsing, drinking through straws, and smoking. If pain is your main concern, you can also review our emergency tooth pain relief guidance for additional comfort tips before your visit. When to call now: if you’re unsure whether a symptom is normal or your discomfort is worsening, contact our Glendale office during business hours for direction.
What to Expect at Your Visit
At your visit, we’ll start with a focused conversation about your symptoms, medical history, and any medications, followed by an exam and X‑rays to pinpoint the source of the problem. We’ll review our findings in plain language, discuss options and comfort steps, and explain what today’s appointment may include. If an extraction is recommended, we’ll outline the steps and your extraction healing timeline so you know what to expect in the coming days.
After we answer your questions and obtain consent, we’ll thoroughly numb the area and confirm you’re comfortable before proceeding; you may feel pressure but not sharp pain. If a tooth needs to be removed, we use careful techniques to free it, clean the site, and place gauze so a protective clot can form. You’ll leave with clear, written after‑care instructions tailored to your case, and we’ll map out check‑ins so you know when and how to contact us during recovery. At home, use gentle pressure with fresh gauze as directed, avoid vigorous rinsing, spitting, or straws the first day, apply a cool compress on the cheek in short intervals for swelling, choose soft foods, and take only dentist‑directed pain relievers as labeled. If the tooth cannot be restored, we’ll review next steps, including emergency tooth extractions, and discuss how we’ll protect the area as it heals. Our team is available during business hours—9:00am–5:00pm Mon–Thurs, and 9:00am–2:00pm Fri—to see you in person here in Glendale and keep you as comfortable as possible along the way. When to call now: contact us immediately during business hours if bleeding stays heavy after 30 minutes of gentle pressure, swelling is worsening quickly, or you notice fever or trouble swallowing.
Home Care Before Your Appointment
If you’re waiting to be seen for a tooth that may need extraction, a few simple steps can help you stay comfortable and protect the area until we examine you. The goal is to manage pain, limit swelling, and avoid further irritation or contamination. These tips are temporary—plan to come in during our business hours so we can evaluate your tooth and discuss next steps.
- Control any oozing by biting gently on clean gauze or a folded, clean cloth for 15–20 minutes; check sparingly and replace if needed.
- Reduce swelling with a cold compress on the cheek: 10 minutes on, 10 minutes off. Avoid heat to the area.
- Keep the mouth clean with gentle swishes of lukewarm saltwater (½ teaspoon salt in 8 oz water) after meals; spit softly and avoid alcohol-based mouthwash.
- Choose soft, cool foods and chew on the opposite side. Skip hard, sharp, sticky foods and very hot drinks that can aggravate the tooth or gums.
- Don’t pick at the tooth or gums, and never place aspirin directly on the tissue. If you use over-the-counter pain medicine, take it only as directed and only if it’s safe for you.
- Avoid smoking, vaping, and alcohol, which can worsen tenderness and bleeding.
We see urgent dental needs in Glendale during business hours (9:00am – 5:00pm, Mon – Thurs, and 9:00am – 2:00pm Fri); call so we can reserve time to evaluate you and take any needed X‑rays. For comfort tips while you wait, you can review our page on emergency tooth pain relief. Starting gentle care now supports the extraction healing timeline once treatment begins. When to call now: if you have facial swelling, fever, trouble swallowing, uncontrolled bleeding after 30 minutes of pressure, or pain that is rapidly worsening.
First Few Days Post-Extraction
The first 24–72 hours are about protecting the blood clot and keeping you comfortable. Expect mild swelling, tenderness, and a small amount of pink-tinged saliva on day one; these are typical early steps in the extraction healing timeline. Rest, keep your head elevated when possible, and avoid anything that could disturb the clot so your body can begin repairing the area. If something feels off, call our Glendale office during business hours (9:00am–5:00pm Mon–Thurs, 9:00am–2:00pm Fri) so we can check you in person.
- Leave the initial gauze in place as directed; if minor bleeding continues, bite gently on fresh gauze for 30–45 minutes.
- Use a cold compress on the cheek 10–20 minutes on/off for the first day to help with swelling.
- Take over-the-counter pain relievers as directed on the label unless your dentist advised otherwise.
- Stick with cool or room‑temperature soft foods; avoid straws, vigorous rinsing, spitting, smoking, or vaping.
- After 24 hours, gently rinse with warm salt water if your dentist advised it; brush and floss the other teeth carefully.
- Limit physical activity for a couple of days and sleep with your head slightly elevated.
Here’s what most people notice: numbness wears off the first day, swelling can peak around 48 hours, and soreness usually begins to ease by day two or three. It’s common for your jaw to feel tight for a short time. If you need more comfort tips, see our emergency tooth pain relief guidance, and contact us during business hours so we can evaluate you in person. When to call now: if bleeding doesn’t slow with firm gauze pressure, pain escalates instead of improving, or you develop worsening swelling, fever, or a bad taste/odor.
Managing Pain and Discomfort
Managing pain and discomfort after a tooth extraction is about protecting the area, keeping swelling down, and using simple, safe measures until the tissues settle. The first 24–48 hours are usually the most tender; after that, soreness should gradually ease as the socket begins to stabilize. Knowing where you are in the extraction healing timeline helps set expectations and prevents overdoing it while you recover. Our team can show you simple ways to stay comfortable while your mouth heals.
For day-one comfort, rest with your head elevated and apply a cold compress to your cheek in short intervals to help limit swelling; avoid heat early on. Take any prescribed medications exactly as directed, or consider an over-the-counter pain reliever you’ve used safely before (never place pills directly on the gums). Keep the blood clot undisturbed: do not smoke or vape, skip straws, and avoid spitting forcefully. Choose cool, soft foods and plenty of water; steer clear of very hot, spicy, hard, or chewy foods. After the first 24 hours, begin gentle warm saltwater rinses after meals to keep the area clean—swish lightly and let it fall from your mouth rather than spitting. Minor oozing is common at first; you can place clean gauze and bite with gentle pressure until it slows. Many people find discomfort begins to improve after a couple of days and continues to settle over the first week; if pain is intensifying or keeping you from resting, we can help with emergency tooth pain relief during our office hours (9:00am – 5:00pm Mon – Thurs, 9:00am – 2:00pm Fri). When to call now: contact our Glendale office during business hours if pain is severe, swelling worsens, bleeding won’t slow with gentle pressure, or you notice fever or a bad taste.
Signs of Proper Healing
Proper healing after a tooth extraction looks like steady improvement, not overnight perfection. Within the first day, a dark red blood clot should fill the socket; light oozing slows, soreness is manageable with rest and a cold compress, and swelling tends to peak around 48 hours before easing. A small amount of pink‑tinged saliva can be normal early on, and any numbness from local anesthetic should fade within a few hours. Mild jaw stiffness or a dull ache that responds to rest and over‑the‑counter medication is typical; most people notice that each morning feels a little better than the day before.
Along the extraction healing timeline, most patients feel noticeable day‑by‑day progress: mild soreness that fades, less need for pain medicine, and easier chewing on the opposite side. Small bruising can be normal; it typically lightens by day three to five. If you were given stitches, they usually dissolve or are removed in about a week, and tissue edges look closed or nearly closed by then. A soft white or yellow layer over the socket is often normal healing tissue, not pus, and the gum edges should look pinker and less puffy as the week goes on. Support healing with simple care: keep the clot undisturbed, avoid smoking and straws, do not rinse or spit forcefully the first 24 hours, then switch to warm saltwater rinses, choose soft foods, and sleep with your head slightly elevated the first couple of nights. By days four to seven, tenderness should keep declining, your breath and taste should normalize, and you can gradually reintroduce more foods as chewing becomes comfortable. If pain suddenly worsens, a bad taste persists, or bleeding doesn’t slow with gentle pressure, call our office during business hours (9:00am–5:00pm Mon–Thurs, 9:00am–2:00pm Fri); for comfort tips, see our emergency tooth pain relief. When to call now: Any increase in pain, swelling, or bleeding after the second day warrants a same‑day evaluation during business hours.
Potential Complications to Watch For
Most extractions heal steadily, but a few warning signs deserve attention so small issues don’t become bigger ones. Along your extraction healing timeline, watch for symptoms that worsen instead of improve or that interfere with eating, sleeping, or opening your mouth. The examples below don’t diagnose a condition; they simply signal it’s time to speak with a dentist promptly during normal office hours.
- Pain that intensifies after the second or third day, feels deep or throbbing into the ear or jaw, or doesn’t ease with over‑the‑counter medication as directed.
- Bleeding that doesn’t slow after 60 minutes of firm pressure with clean gauze, or bleeding that restarts repeatedly when you sit up or move around.
- Swelling that enlarges after day three, spreads toward the eye or neck, or comes with fever or chills.
- Numbness or tingling in the lip, chin, or tongue that lasts beyond the immediate post‑procedure period or seems one‑sided.
- Pus, a foul taste, or persistent bad breath coming from the extraction area.
- After upper back teeth: liquid passing from mouth to nose when drinking, air bubbling through the socket, or sinus pressure that worsens.
If any of these occur, keep gentle pressure with fresh gauze for 20–30 minutes to help control bleeding, apply a cold compress up to 20 minutes at a time during the first day, and use over‑the‑counter pain relievers only as directed unless your physician has advised otherwise. Avoid straws, vigorous rinsing, or tobacco so the clot can stabilize; after the first 24 hours, warm salt‑water swishes after meals can help keep the area clean without disturbing healing. Then contact our Glendale office during business hours—9:00am – 5:00pm Monday–Thursday and 9:00am – 2:00pm Friday—so we can assess the site and advise next steps. If pain is your main concern, you might find quick tips on our page about emergency tooth pain relief while you arrange a visit. When to call now: worsening pain, persistent bleeding, spreading swelling, fever, or any concern that you’re not improving day by day.
Nutrition During the Healing Process
What you eat after a tooth extraction directly affects comfort and how well the blood clot stays protected. For the first couple of days, choose soft, cool, nourishing foods and drink plenty of fluids so you stay hydrated without disturbing the area. Skip straws, alcohol, and very hot, spicy, or crunchy foods early on, as they can irritate the site. Everyone heals at a different pace, but your extraction healing timeline is supported by gentle, steady nutrition.
During the first 24 hours, focus on smooth, cool or room‑temperature options like applesauce, mashed bananas, smooth soups (cooled), mashed potatoes, scrambled eggs, and protein-rich smoothies eaten with a spoon instead of a straw. Take small sips of water throughout the day; avoid carbonated drinks and alcohol. On days 2–3, if you’re comfortable, add soft, lukewarm foods such as tender pasta, flaky fish, well‑cooked vegetables, and oatmeal without seeds or crunchy add‑ins. Chew on the opposite side, keep textures soft, and stop any food that causes throbbing or sensitivity. Avoid small seeds, chips, crusty bread, and spicy or acidic items until tenderness clearly improves. Starting 24 hours after your procedure, a gentle lukewarm saltwater rinse after meals can help keep the area clean without vigorous swishing. If pain spikes or lingers sharply with hot or cold, review our guidance for emergency tooth pain relief and plan an in‑person visit during our business hours (9:00am–5:00pm Mon–Thurs, 9:00am–2:00pm Fri) so we can evaluate you in Glendale. When to call now: contact us during business hours if you cannot keep fluids down, bleeding doesn’t ease with gentle pressure after about an hour, or your discomfort is worsening instead of settling.
Maintaining Oral Hygiene After Extraction
Cleanliness matters after a tooth is removed, but it has to be gentle so you don’t disturb the blood clot that protects the socket. For the first 24 hours, avoid rinsing forcefully, spitting, or using a straw, and keep your tongue and fingers away from the socket so the clot can stabilize. Starting the next day, use warm saltwater swishes to freshen your mouth and lower bacteria without stinging. These habits support your extraction healing timeline and reduce the chance of irritation.
Use a soft-bristled brush; angle the bristles away from the socket and clean the chewing surfaces normally. Floss as usual but skip the empty space until your dentist clears you. Choose soft foods and chew on the opposite side so debris doesn’t pack into the site; if food collects, let it soak loose with saltwater rather than picking at it. After 24 hours, a gentle rinse recipe is 1/2 teaspoon of table salt dissolved in a cup of warm water, swished for 20–30 seconds after meals. Avoid alcohol-based mouthwashes and peroxide for several days, and do not smoke or vape, which can dry the area. Stay hydrated and keep your lips and cheeks relaxed—suction and vigorous swishing can dislodge the clot. Remove partials, retainers, or aligners unless you were told to wear them continuously; clean them outside your mouth before reinserting. If discomfort is hard to manage or tooth pain elsewhere is flaring, see our emergency tooth pain relief page for what to expect and call our Glendale team during business hours (9:00am – 5:00pm, Mon – Thurs, and 9:00am – 2:00pm Fri) for guidance. When to call now: contact us during business hours if bleeding continues despite gentle pressure, swelling increases, you notice fever or a bad taste/odor, or pain worsens instead of easing after the second day.
Follow-Up Appointments Importance
Follow-up appointments matter because they let your dentist confirm your socket is closing and the gum tissue is healing as expected, remove stitches if needed, and make small adjustments to keep you comfortable. They also help verify your bite and neighboring teeth are not stressed while you recover, and that your pain control plan is appropriate. These check-ins keep your extraction healing timeline on track and reduce the chance of avoidable setbacks.
At these visits, we examine the area visually, gently irrigate if appropriate, and may take a quick x-ray to confirm bone and socket changes are progressing normally. If sutures were placed, we remove them when the tissue is ready, and we’ll update your home-care plan—such as when to begin saltwater rinses, how to brush near the site, and which foods are easiest while you heal. We also check your bite and the adjacent teeth, review any medications you’re taking, and answer questions about returning to work, exercise, or travel. Between appointments, keep the area clean with light rinsing as directed, avoid straws and smoking until you’re cleared, and use only over-the-counter pain relievers as labeled unless we’ve advised otherwise. If discomfort spikes between visits, our page on emergency tooth pain relief explains what an in‑office evaluation involves during business hours. Please schedule or adjust follow-ups with our Glendale team during 9:00am – 5:00pm, Mon – Thurs, and 9:00am – 2:00pm Fri; timely check-ins help prevent small issues from becoming bigger problems. When to call now: worsening pain, facial swelling, persistent bleeding, fever, or a bad taste/odor from the area should be reported during business hours so we can advise you and arrange the next visit.
Frequently Asked Questions
Here are quick answers to common questions people have about Tooth Extraction Healing Timeline in Glendale, AZ.
- What should I expect in the first 24 hours after a tooth extraction?
In the first 24 hours after a tooth extraction, it’s crucial to protect the blood clot that forms in the socket. You should rest, keep your head elevated, and avoid spitting or using straws. Bite gently on clean gauze to control any bleeding and manage swelling with a cold compress applied to your cheek. Stick to soft, cool foods and small sips of water. Minor oozing and tenderness are normal during this time.
- When should I contact a dentist after a tooth extraction?
Reach out to a dentist if pain worsens instead of improving, if bleeding continues or restarts after 30–60 minutes of pressure with gauze, or if you experience increasing swelling, fever, or a bad taste. Persistent issues or symptoms that appear to worsen rather than improve should be evaluated promptly during business hours. Our Glendale office is available to assist you Monday through Friday.
- Is it normal to feel numbness or tingling after an extraction?
Numbness in the lip, chin, or tongue is common immediately after a tooth extraction due to the local anesthesia. However, if numbness or tingling persists beyond the first day or feels one-sided, contact a dentist. It’s essential to have such changes assessed to ensure proper recovery and address any potential nerve irritation or damage.
- What foods are safe to eat during the healing process?
During the first couple of days following an extraction, opt for soft, cool, and nourishing foods. Examples include applesauce, mashed potatoes, scrambled eggs, and protein-rich smoothies (skip the straw). Avoid spicy, hot, or crunchy foods that may disturb the extraction site. Gradually introduce soft, lukewarm foods as comfort improves, always chewing on the opposite side.
- How can I manage swelling after a tooth extraction?
To manage swelling, apply a cold compress to your cheek in 10-minute intervals during the first 24 hours. Keep your head elevated while resting to help reduce swelling. Avoid using heat on the extraction area, as it may increase swelling. Light swelling and bruising are normal and usually peak within the first 48 to 72 hours before starting to diminish.
- Can smoking affect my healing process after extraction?
Smoking can significantly impact the healing process following a tooth extraction. It may disturb the blood clot, increase bleeding, and prolong soreness, jeopardizing recovery and raising the risk of infections. To support proper healing, avoid smoking or vaping for at least several days post-extraction or until your dentist advises it is safe to resume.
- How will I know if my extraction site is healing properly?
Signs of proper healing include a gradually improving soreness, less need for pain medication, and a clot that stays in place. By the end of the first week, gum tissue should begin closing over the socket. If you experience unexpected pain or symptoms, contact us during business hours. Improvement typically occurs daily; any setbacks should be promptly addressed.
Medical sources (PubMed)
- Carrasco-Labra A, et al. JADA. 2024. “Evidence-based clinical practice guideline for the pharmacologic management of acute dental pain in adolescents, adults, and older adults: A report from the American Dental Association Science and Research Institute, the University of Pittsburgh, and the University of Pennsylvania.”. PMID: 38325969 / DOI: 10.1016/j.adaj.2023.10.009
- Carrasco-Labra A, et al. JADA. 2023. “Evidence-based clinical practice guideline for the pharmacologic management of acute dental pain in children: A report from the American Dental Association Science and Research Institute, the University of Pittsburgh School of Dental Medicine, and the Center for Integrative Global Oral Health at the University of Pennsylvania.”. PMID: 37634915 / DOI: 10.1016/j.adaj.2023.06.014
- Mathis J, et al. J Vet Dent. 2025. “Oral and Dental Pain Management.”. PMID: 39311042 / DOI: 10.1177/08987564241279550
- Cope AL, et al. Cochrane Database Syst Rev. 2024. “Systemic antibiotics for symptomatic apical periodontitis and acute apical abscess in adults.”. PMID: 38712714 / DOI: 10.1002/14651858.CD010136.pub4
- Pigg M, et al. J Endod. 2021. “New International Classification of Orofacial Pain: What Is in It For Endodontists?”. PMID: 33340605 / DOI: 10.1016/j.joen.2020.12.002
- Pergolizzi JV, et al. Expert Opin Pharmacother. 2020. “The pharmacological management of dental pain.”. PMID: 32027199 / DOI: 10.1080/14656566.2020.1718651